What Are the Four Main Aims of PSIRF?
The Patient Safety Incident Response Framework (PSIRF) is pivotal in enhancing patient safety within healthcare settings. Understanding its main aims can significantly improve how healthcare providers respond to patient safety incidents.
So, What Are the Four Main Aims of PSIRF?
1️⃣Compassionate engagement and involvement of those affected by patient safety incidents
2️⃣Application of a range of system-based approaches to learning from patient safety incidents
3️⃣Considered and proportionate responses to patient safety incidents
4️⃣Supportive oversight focused on strengthening response system functioning and improvement
Let’s explore these essential objectives in more detail ⬇️
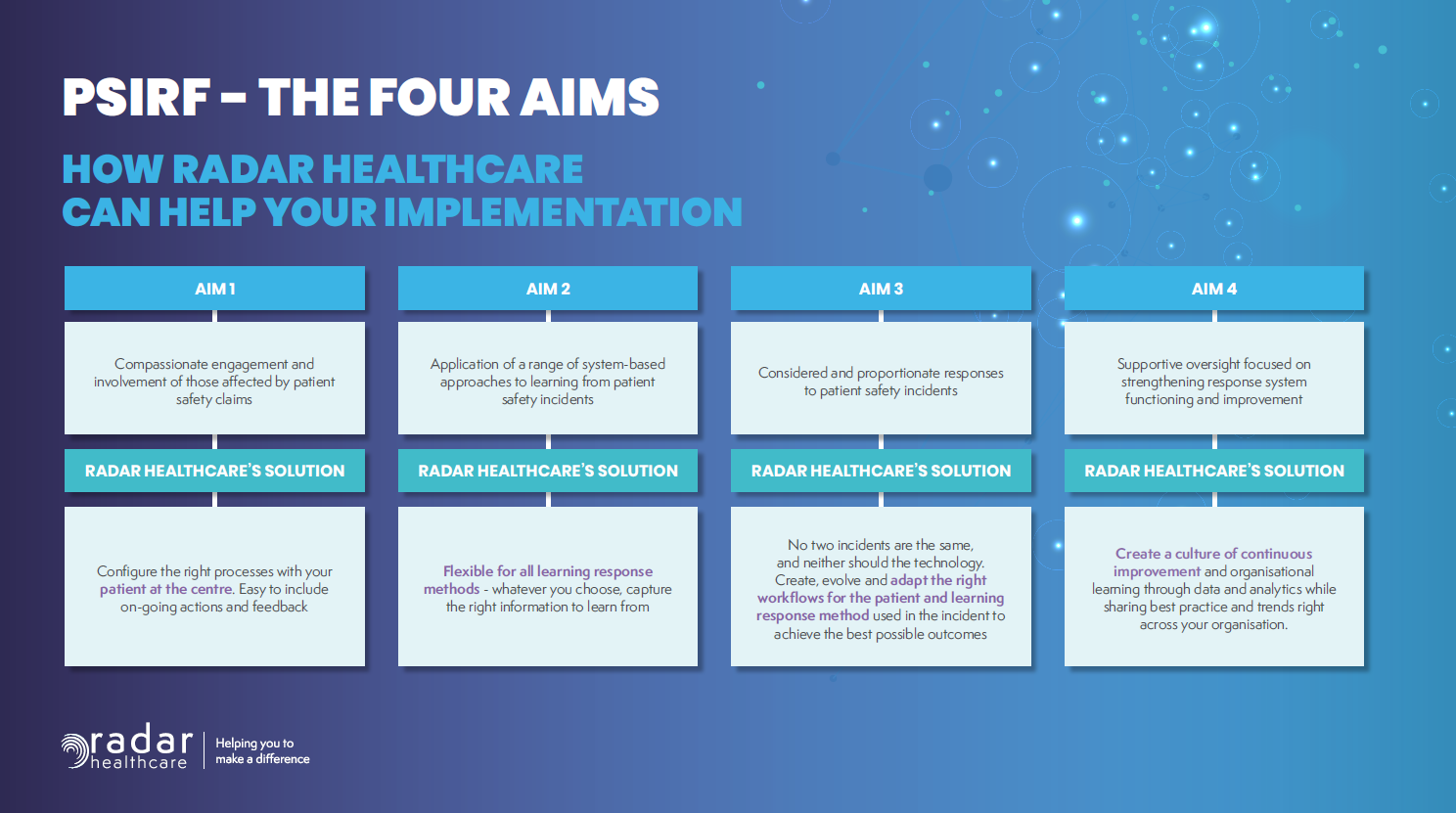
The 4 Main Aims of PSIRF Explained
PSIRF Aim 1️⃣: Compassionate engagement and involvement of those affected by patient safety incidents
Learning from a patient safety incident can only happen if there are processes put in place to support the compassionate engagement and involvement of those affected, including patients, their families and staff.
This means creating safe spaces and opportunities for discussion, understanding and for asking questions that all parties may have in relation to the incident.
When a patient safety incident investigation (PSII) occurs, patients, their families and staff should be engaged in a meaningful way – but only if they want to.
PSIRF Aim 2️⃣: Application of a range of system-based approaches to learning from patient safety incidents
The PSIRF will be encouraging the use of system-based approaches to patient safety incidents, instead of more linear methods of identification.
Organisations will be asked to use the national learning response tools and guides to understand and uncover contributing factors to a patient safety incident, or incidents, to drive improvements.
Those who lead the patient safety incident responses and those involved in the learning and improvement from these responses will need specific knowledge and experience, details in official standards.
PSIRF Aim 3️⃣: Considered and proportionate responses to patient safety incidents
The goal of the PSIRF is to maximise improvement, not to reach a particular threshold of patient safety incident responses. Each organisation has a finite number of resources, and they must expend those resources in a way that benefits them and their outreach.
Some incidents like ‘Never Events’ and deaths require a PSII to understand the actions behind that incident and where improvements and learnings can be made. Similarly, certain incidents need to follow specific reporting and reviewing processes, which are detailed in the guide.
The PSIRF aims to put accountability and responsibility back into the hands of the organisations. If an organisation or Trust and its ICB are satisfied with the response to an incident, it will be acceptable to forego further action.
PSIRF Aim 4️⃣: Supportive oversight focused on strengthening response system functioning and improvement
Organisations must work collaboratively, understanding their shared aims of the PSIRF. An effective governance structure is expected, with ICBs required to facilitate that collaboration at both place and system levels.
The PSIRF also expects ICBs and other regulators to understand and evaluate the effectiveness of NHS providers’ response processes. The leaders of the providers are accountable for the quality of learning responses, not the providers themselves.
However, providers should be open with the information relating to patient safety incidents and incident responses, as well as support the continuous development of the framework. More information about this is available in ‘Oversight roles and responsibilities specification’.
Implementing PSIRF in your organisation
To effectively implement PSIRF, healthcare organisations should commit to these four aims. Here are some practical steps:
👨💼 Leadership Commitment: Ensure that leaders prioritize patient safety and actively support PSIRF initiatives.
📚 Comprehensive Training: Offer regular training sessions for all staff members on PSIRF principles and practices.
🔍 Clear Reporting Channels: Establish transparent and accessible channels for reporting patient safety incidents.
📊 Regular Evaluations: Conduct periodic evaluations to assess the effectiveness of PSIRF implementation and make necessary improvements.
"Patient safety and quality of healthcare are paramount to the LivingCare Group. We needed a solution that could meet the Patient Safety Incident Response Framework (PSIRF) and Learning From Patient Safety Events (LFPSE) standards, and Radar Healthcare provided the perfect solution.”

How technology plays a part
Having the right systems in place is a huge part of improving patient safety because data and analytics from previous incidents is the key to learning how to avoid these in future.
Radar Healthcare is a risk, quality and compliance system built with patient safety in mind. LFPSE compliant and packed with AI, the software helps you accurately log incidents, put in place action and improvement plans, and report on improvements made. Book a demo below.
Summary
Understanding and integrating the four main aims of PSIRF can significantly enhance patient safety in healthcare settings. By fostering a culture of safety, improving systems, empowering staff, and committing to continuous learning, healthcare organisations can create a safer environment for both patients and staff.
"We had a fantastic reporting team that greatly contributed to the successful implementation of Radar Healthcare and LFPSE. Sarah Adams from Radar Healthcare served as our Project Manager and maintained constant communication with us. She fostered a strong relationship with our team, making it easier to progress and align with our internal goals, as well as align with national directives like LFPSE and PSIRF."